
April’s Topic of the Month – Coping with Oral and Nasal Ulcers
 May 03rd, 2017
May 03rd, 2017 Nakita Cambow
Nakita Cambow Blog
Blog 0 Comments
0 Comments
Oral (mouth) and nasal (nose) ulcers are one of the most common features of lupus occurring in around 45% of people who have SLE. Having mucosal ulcers in the mouth or nose is one of the classification criteria used to diagnose SLE. Ulcers can be painful and uncomfortable.
What causes ulcers?
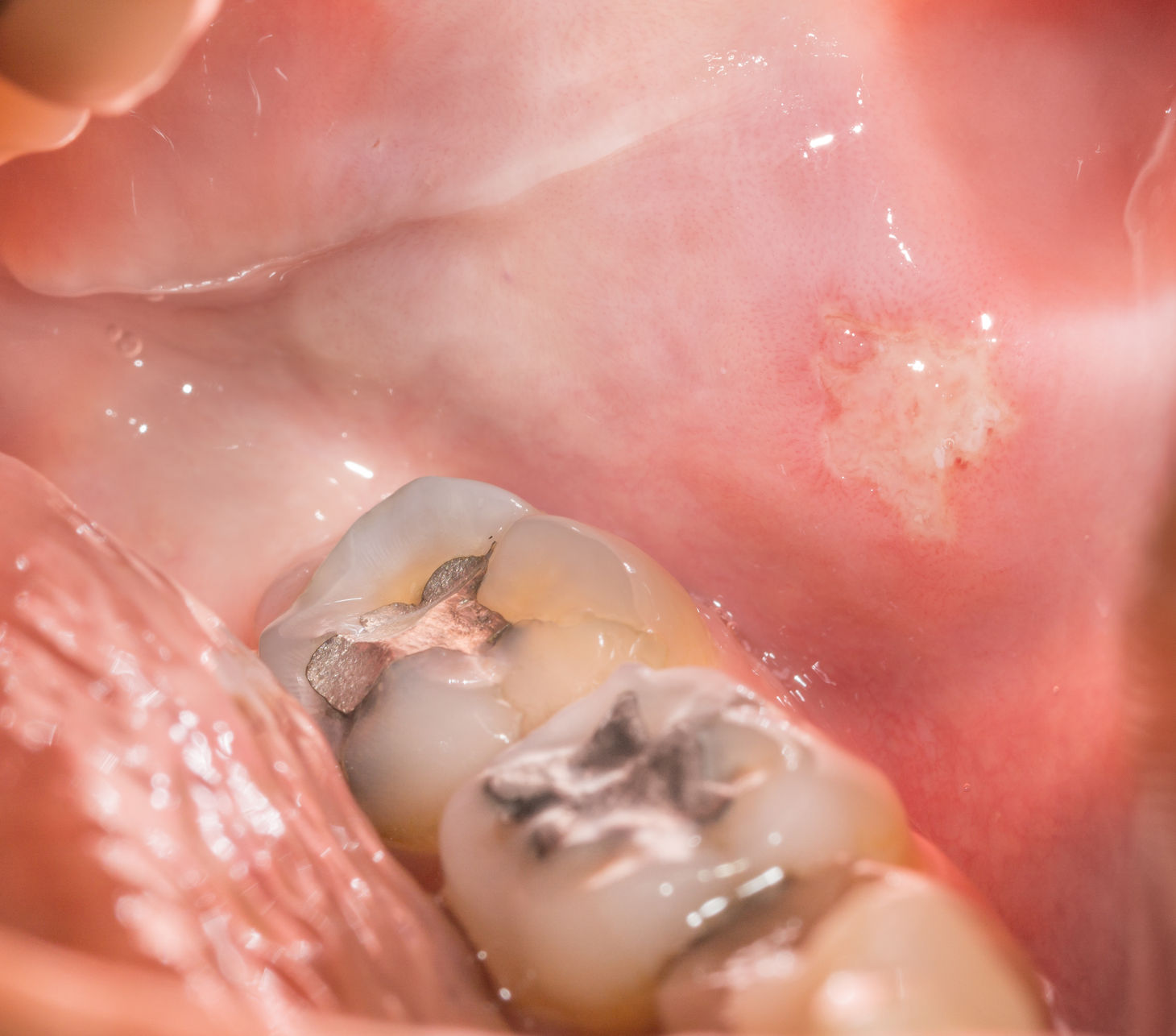 Mouth and nose ulcers often occur during lupus flares and may be associated with joint pains, rashes and hair loss. Fortunately when the disease settles, the mouth ulcers settle as well in most people, although stress or tiredness can make the mouth ulcers worse.
Mouth and nose ulcers often occur during lupus flares and may be associated with joint pains, rashes and hair loss. Fortunately when the disease settles, the mouth ulcers settle as well in most people, although stress or tiredness can make the mouth ulcers worse.
“I get the mouth ulcers frequently with a flare – they will appear as one of my first symptoms of a flare (the ‘uh oh’ moment, here we go again). I have mostly had them toward the base of the tongue or back of the mouth at the gum line and those have always been very painful”
Ulcers are open sores where the overlying skin has eroded away, leaving tissue beneath the skin surface exposed. These can occur in the mucosa of people who have SLE. The mucosae (plural of mucosa) are lubricated skin surfaces such as the areas found inside the mouth, nose, and vagina.
Oral ulcers can occur anywhere inside the mouth, but most commonly they develop on the roof of the mouth. Another term used for mucosal ulcers, especially when there is widespread inflammation, is “mucositis”. Sometimes these sores can spread to the lips as well. This primarily occurs in people who become very sick with their SLE when it is affecting other major organs (such as the kidneys) and is often accompanied by fever.
Nasal ulcers typically occur on the septum (the wall dividing the right and left nostrils) or on the mucosal skin covering the thick centre cartilage of the nose.
The most common form of mouth ulcer is an ‘aphthous’ mouth ulcer. At least 1 in 5 people can develop aphthous mouth ulcers at some stage in their lives and they are therefore not specific to lupus and can have many potential causes. Whilst people with lupus may also develop these, mouth ulcers caused by lupus are a different type.
Most aphthous mouth ulcers are caused by things you can try to avoid, such as:
- biting the inside of your cheek
- badly-fitting dentures, braces, rough fillings or a sharp tooth
- cuts or burns while eating or drinking – for example, hard food or hot drinks
- a food intolerance or allergy
- damaging your gums with a toothbrush or irritating toothpaste
–
Sometime they’re triggered by things you can’t always control, for example:
 feeling tired, stressed or anxious
feeling tired, stressed or anxious- hormonal changes (such as during pregnancy)
- your genes (some families get mouth ulcers more often)
- an overlapping condition (such as inflammatory bowel disease (IBD), coeliac disease or Behçet’s disease)
- a vitamin B12 or iron deficiency
- certain medications (including some NSAIDs, beta-blockers or nicorandil)
–
If you believe stress/anxiety could be the cause of your ulcers, you may find our previous blog article about Stress Management and Relaxation helpful. You can read it HERE.
If you suspect that your ulcers could be caused by a nutritional deficiency such as vitamin B12 or iron, you could ask your doctor for blood tests and possibly dietary supplementation. It is advised to always discuss any dietary supplements with your doctor first if you have lupus.
What treatments are available?
From your doctor
Medicines used by doctors to control SLE such as steroid tablets (prednisolone) and anti-malarials (hydroxychloroquine) usually help to decrease the severity of the mucositis outbreaks. Sometimes using local applications of steroids can also be useful. If this is done as soon as they occur and then used every few hours, it can help the sores to heal faster than usual. For particularly painful oral ulcers, an anaesthetic (benzocaine) in Orabase can decrease the discomfort. Likewise, steroid nasal sprays or steroid pastes can be used for nasal ulcers. These can be prescribed by a doctor.
“Any time I’ve been on an immune modulating medications or biologics I’ve had far fewer ulcers – a welcome relief if you can find a med that works for you.”
“I’ve not had so many since I’ve been taking hydroxychloroquine.”
 “I have a steroid inhaler for asthma. I spray this on my mouth ulcers (doctor’s advice) and now they last three days instead of three weeks. This is only effective on ulcers that you can get to though.”
“I have a steroid inhaler for asthma. I spray this on my mouth ulcers (doctor’s advice) and now they last three days instead of three weeks. This is only effective on ulcers that you can get to though.”
“For large or unresponsive mouth ulcers my GP prescribes hydrocortisone 2.5 mg buccal mucosal pellets. The steroid reduces pain to allow me to eat.”
“My dermatologist prescribed me betamethosone dipropionate gel, augmented, 0.05%. Because of the gel formulation it sticks around longer, coats the ulcer, soothes and the steroid helps heal. I tried multiple over-the-counter products without any real relief.”
“I felt like I tried everything available over-the-counter and home remedies etc without much real success until my periodontist recommended Gengigel products several years ago.”
“Naseptin always works a treat for my nose sores/ulcers.”
“I struggle with nasal sores. They are so bad they sometimes break through to the outside of my nose; it looks and feels awful. I’ve been prescribed Naseptin but it’s not great; it can still take weeks for them to heal and then it’s never more than a few days before a new one comes back.”
“My ENT first recommended NeilMed treatments to me a few years ago. Used regularly, NeilMed treatments really help prevent my lesions and ulcers and when these do crop up they’re less severe….it’s as if NeilMed sprays, rinses, gels etc. seem to help prevent my nose ulcers becoming infected and make healing faster.”
“My nose ulcers tend to get infected. Then prescription topical antibiotics are the only solution. At first I was prescribed Naseptin, but after a few years I became resistant to that, so now I’m prescribed bactroban: this still works!”
Over-the-counter
Your pharmacist can recommend some suitable treatments that may help to speed up healing, prevent infection or reduce pain, for example:
- antimicrobial mouthwash
- a painkilling mouthwash, gel or spray
- corticosteroid lozenges
–
You can buy these without a prescription, but they may not always work. It is very important that you read the package instructions thoroughly. Also, check with your doctor first to make sure the medicine is safe to use in light of any other medical problems you may have, and to ensure it is safe to use with your other medications. Never take over-the-counter medicines without doing this first; otherwise there is always the potential risk of drug interactions.
“I can recommend Difflam mouthwash and Bonjela for mouth ulcers. The mouthwash has a steroid in it and if used before meals can help with the pain of eating! It shouldn’t be used for more than a week at a time because of the steroid. You can get it on prescription or buy it, but it’s very expensive!”
“Difflam spray really helps me. I get clusters of excruciating ulcers in the folds at the back of my throat/tongue and I can carry it in my handbag. Vaseline for my nose always does the trick.”
“The nasal ulcers do stay away better, I believe, with frequent use of a nasal saline spray. The salt water helps hydrate (to overcome the sicca symptoms) and keep the pH balanced. I also have to use a topical antibiotic if they take off; usually I use a dab of polysporin a couple of times a day for a few days.”
“I tend to use warm water Himalayan salt mouth wash and Anbesol or Bonjela to numb the pain, especially before eating.”
“My mouth ulcers are less frequent since I started using Corsodyl toothpaste (not the gel one though). The toothpaste tastes cack but it’s worth it for fewer ulcers.”
“I use Corsodyl mouthwash when I feel mouth ulcers coming. Having Sjögren’s I know how important oral health is, so I always keep on top of regular dental checks. I never rinse, use strong fluoride toothpaste, and also use saliva stimulation if I have a dry mouth, as saliva will naturally keep bacteria under control.”
“I’ve had great success using red light therapy to heal mouth ulcers. I use the MouthUlcerClear Advance from Lloyds Pharmacy. It’s a small wand with red light at the tip which is held against the ulcer. In most cases the ulcer is gone overnight.”
“Tyrozet lozenges have antiseptic and anaesthetic, they help to numb your ulcers.”
“I get loads of mouth ulcers. I use cortisone pellets depending where they are; if I can place it on the ulcer they are gone quickly.”
“I get intermittent pain relief with a topical anaesthetic oral gel from Boots which contains lidocaine 2%. This helps at meal times as eating can be painful.”
“I find chewing cabbage deals effectively, and quickly, with oral ulcers…. even large, multiple ones.”
“I always put a bit on Vaseline up my nose over the sore. It really helped as they didn’t have painful crusts then and were a lot less painful.”
When should I seek help from a doctor?
It is important to make an appointment with your GP or dentist if an ulcer lasts longer than three weeks or becomes more painful and red, as this may be a sign of an infection. Although most mouth ulcers are harmless, a long-lasting mouth ulcer is sometimes a sign of mouth cancer. It’s best to get it checked.
“If you get a cluster of mouth ulcers at any one time it’s worth talking to your medical team about them because they can be a sign of a flare or a side effect of the immunosuppressives!”
Is there anything I can do to prevent mouth ulcers developing?
Avoiding things that irritate your mouth ulcer should help to reduce pain, speed up the healing process and reduce the chance of it returning. Here are some tips;
- use a soft-bristled toothbrush

- drink cool drinks through a straw
- eat softer foods
- get regular dental check-ups
- eat a healthy, balanced diet (for tips on this, click HERE)
- avoid very spicy, salty or acidic food
- don’t eat rough, crunchy food, such as toast or crisps
- don’t drink very hot or acidic drinks, such as fruit juice
- don’t chew gum
- avoid toothpastes containing sodium lauryl sulphate (SLS)
- If you smoke, give up or at least cut down (this may trigger ulcers in the short term, but you should see an improvement in the long run)
–
“My mouth has improved massively since switching to Sensodyne Pro (it’s one of the only SLS free toothpastes available). I also use Genigel mouthwash which has been proven to aid natural healing and is not as harsh as others.”
“Salty and spicy foods definitely irritate ulcers once I have them.”
“I find a cool, softer diet helps as hot food and liquid irritates my mouth. Ice lollies and yoghurts are soothing. I sip cold water to keep my mouth moist. I also avoid spicy or hard textured food.”
“I gargle salt water three times a day (after food and cleaning teeth). This seems to have reduced the amount of flare-ups I’m having.”
You may find that a change in your diet could help to decrease the likelihood of developing mouth ulcers. Certain foods have been identified as increasing the risk of developing mouth ulcers in some people. These include;
–
Individuals are likely to find that different foods could be triggering mouth ulcers. A way to identify any potential culprits is to keep a food and symptom diary for a number of weeks. Allergy UK has a simple diary that you can print HERE.
“Tomatoes and some other fruits or anything with strong flavours can bring out ulcers on my tongue or the roof of my mouth but they can go away again after a couple of hours.”
“Spicy and sweet food gives me mouth ulcers.”
***Please note that this article is written for informational purposes only and should not be a substitute for professional medical advice or treatment. Do not delay seeking or disregard medical advice based on information here. Always seek the advice of your local family physician or other qualified health professional before starting any new treatment or making any changes to existing treatment. It is also advisable to consult a medical professional before making any changes to diet or starting complementary remedies, which may interact with other medications.***
Thank you so much to everyone who submitted their tips and experiences for this month’s topic. We’re sorry if we weren’t able to use your comment in the article this time.




 ©2024 LUPUS UK (Registered charity no. 1200671)
©2024 LUPUS UK (Registered charity no. 1200671)