Chimeric Antigen Receptor T-cell therapy (CAR-T) has previously shown positive results in treating blood cancers. Based on how this treatment works, efforts have turned towards exploring their potential in treating autoimmune diseases like lupus.
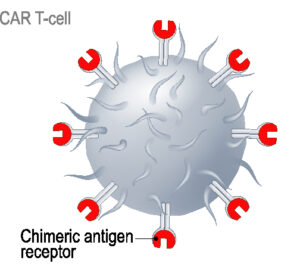
What is CAR-T cell immunotherapy?
“CAR-T cell therapy” stands for “Chimeric Antigen Receptor T-cell therapy” and is a type of immunotherapy.
The immune system has lots of different types of cells, including T cells and B cells. B cells produce antibodies that signal to other parts of the immune system, such as T cells, to destroy infections, disease, and damaged cells. In lupus, the B cells produce autoantibodies which means the immune system mistakenly attacks the body’s own tissues.
CAR-T cell therapy involves collecting a patient’s T-cells and modifying them so that they can recognise and destroy B cells. The idea is that the T cells could destroy the B cells that create the autoantibodies, so the immune system stops attacking the body’s own tissues, which reduces the inflammation and damage caused by lupus.
It’s called “CAR-T cell therapy” because the modification adds receptors to the T cells called “chimeric antigen receptors” or “CAR”. These help the T cell to recognise the B cells they need to destroy.
What happens during CAR-T therapy?
There are usually four main stages to CAR-T therapy treatment:
1. Your white blood cells are collected. This is called “leukapheresis”. These cells are then used to make your CAR-T treatment, which can take a few weeks.
2. A few days before your treatment, you have “lymphodepletion”, which is the process of reducing the number of white blood cells in your body to make “space” for the CAR-T treatment. Sometimes this is referred to as “conditioning treatment”, and you may also hear it called “chemotherapy” because some of the drugs used in lymphodepletion are also used in chemotherapy.
3. The CAR-T treatment is given as a one-time infusion in hospital.
4. You need to stay in and nearby the hospital for monitoring. You may need to stay in the hospital for between 10 to 30 days, but this will vary depending on the specific trial and how you respond to the treatment.
After the treatment, you would continue to be monitored, often including blood tests and questionnaires. As part of a clinical trial, you would be told what monitoring would be needed afterwards, and how often, before you agreed to take part.
CAR-T therapy and lupus
A small clinical trial in 2022 tested CAR-T therapy with five people with severe SLE. All five people experienced remission of their lupus and were able to withdraw from their lupus medication for between three and seventeen months. This was a very promising and exciting result. However, this was a very small study, so more research needs to be done with more people to see if it is safe and effective and, if so, who it might be most effective for.
There are clinical trials starting or starting soon for CAR-T therapy for people with lupus and other autoimmune disease in the UK.
Are there any risks or side effects of CAR-T therapy for people with lupus?
There is not enough research yet, so it is not clear what the side effects or risks may be for people with lupus. We will know more as more research reports results and when there has been longer follow-up of participants from current trials.
From the 2022 study of people with lupus and experience from its use in blood cancer, some potential side effects include:
- Allergic reactions during the infusion
- Low blood cell counts
- A weakened immune system
- Complications of the nervous system
Some trials may also require a person to stop taking certain lupus medications during the process, which may risk a flare-up.
If you took part in a trial of CAR-T, any risks should be discussed with you clearly so that you understand before you agree to take part.
Will CAR-T therapy work for all people with lupus?
There is not enough research yet. The larger trials with more people are needed to confirm that the treatment is safe and effective for people with lupus, and to see if there are particular people it is most effective for. As lupus can impact people differently, it may be that it is not effective for everyone or for all types of lupus. It is not clear yet whether there are specific patient characteristics that impacts how people respond to CAR-T.
Is CAR-T therapy available in the UK for lupus?
This type of treatment is used for some types of blood cancer in the UK. You can find out more information about CAR-T therapy as a blood cancer treatment on Cancer Research UK’s website.
It is not available as a treatment for any other condition, including lupus, in the UK.
There are clinical trials starting or starting soon for CAR-T therapy for people with lupus and other autoimmune disease in the UK. Only people who lupus who are participating in a trial can receive CAR-T therapy.
Can I take part in a clinical trial? Where do I find out about clinical trials for lupus?
Usually, you cannot refer yourself or contact the trial team yourself, and you have to be referred by your doctor. If you are interested in taking part in a trial, or you want to find out what trials are happening in lupus near you, you can:
- Speak to your rheumatologist and say you are interested in clinical trials.
- Sign up to our e-newsletter and keep an eye on our website to stay updated on the latest information about this therapy and other trials in lupus.
- Search for “lupus” on the Be Part of Research website (note: this doesn’t include all trials for lupus).
You can also find out more about the different types of clinical trial and ways to take part on the NHS website.
Trials all have “eligibility criteria”, which means that only people with certain characteristics, such as particular symptoms, are able to take part. Different trials can have different eligibility criteria.
When will CAR-T therapy for lupus be available on the NHS?
CAR-T is not likely to be available on the NHS soon.
The research is still in early stages, so it is not possible to say, but it likely to be some time. Before it can be made available for more people, there needs to be more research to check it is safe, effective, and who it is safe and most effective for. If the research has positive results, it will then need to go through NHS approval processes. If the research does not have positive results, then it is unlikely to go through the NHS processes and become available.
What happens next for CAR-T and lupus?
While CAR-T cell therapy shows promising potential for treating lupus, it’s important to understand that this research is still in its early stages. So far, only a small number of people with severe or treatment-resistant lupus (cases where other therapies haven’t worked) have participated in these studies. The therapy has shown positive results in this limited group, providing hope for patients who don’t respond well to conventional treatments.
However, more research is needed to confirm its effectiveness and safety in a broader population. Not all people with lupus may be eligible or benefit from CAR-T therapy, especially those with milder forms of the disease. Larger clinical trials are essential to determine if this therapy can work reliably and safely across different types and stages of lupus. If these trials succeed, CAR-T therapy could represent a significant breakthrough for lupus treatment. But until more data is gathered, it is not clear how effective it is for people with lupus. It will not be available as a treatment until this research is done.

